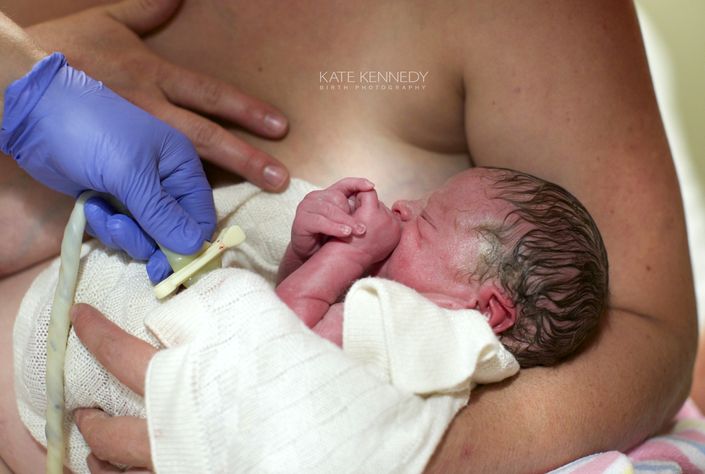
Neonatal Stabilisation with an Intact Cord
Physiological transition with optimal cord clamping
Watch Promo
Welcome change agents
This exciting new online course is the first ever online module dedicated to the education and practice of stabilisation of the newborn at birth with an intact umbilical cord.
We use the developing research knowledge base around optimal cord clamping to provide you with new insight, detailed practical application and strategies to help facilitate change to practice at your place of work.
This course has a global context as it discusses bedside stabilisation strategies in varying practice settings, from low tech birth locations where resources are sparse to high tech environments where challenges to practice change can be equally problematic.
This module is relevant to:
- All midwifery practitioners and students
- Obstetricians and Neonatologists
- Anaesthetists and Operating Department Practitioners
- Medical trainees
- Governance and guideline professionals
We have approached this module considering the high-level problem statements practitioners share when trying to change practice to optimal cord clamping and further resuscitation with an intact cord. We aim to provide answers to the problems you’re facing and present the structured guidance needed to support practice change.
Education
The first two chapters concentrate on physiology and the benefits of blood volume transition in order to improve practitioner knowledge of neonatal adaptation to extrauterine life.
Perspective
Chapters three, four and five explore the advantages and challenges to practising bedside stabilisation in various clinical settings.
Solutions
Chapter six looks at strategies for change management; detailing how to go about implementing intact cord stabilisation within your areas of work. We provide a quick-fire myth busting chapter which we hope will help you to overcome common challenges you might encounter from others who may not understand the evidence for physiological based transition.
How the module works
The module is made up of author audio presented videos and occasional text chapters to read, although we understand this might not suit all learning preferences, we have done our best to make this as engaging as possible.
Please start at Chapter 1 and work through in chronological order and the learning builds as you progress the module.
Following each chapter there are a set of graded questions to answer. These questions will help you to cement key principals and reflect on your learning. You are required to get 100% in each quiz but can retake each quiz as many times as needed.
You will need:
- A quiet space or access to a set of headphones
- A notepad
You will be provided with a graded certificate on completion of the module which can be used towards professional revalidation.
Tips
The course takes approximately an hour, however if you are unable to complete it in one go, the platform will automatically save your progress at the end of each section. The progress bar on the left of the curriculum screen will guide you.
If you skip the videos the course will not update your percentage completion and you will need to go back to watch the videos in order to get your certificate.Please find the full course curriculum below and we hope you enjoy learning.
Your Instructors

Hannah Tizard
Hannah is a registered midwife and midwifery educator at the University of Central Lancashire.
Holding the strong evidence base for optimal cord clamping in high regard Hannah is keen to support change in practice, believing it is a fundamental right for all babies, especially those who may be born in poor condition, pre-term and by caesarean section.
Hannah founded the BloodtoBaby campaign in 2015 to raise global awareness about optimal cord clamping through dissemination of materials and education. She has had materials for Optimal Cord Clamping endorsed by the National Institute for Health and Care Excellence (NICE) and because of this work won the Royal College of Midwives Evidence into Practice Award in 2016.
Hannah is responsible for building a team of multi-disciplinary professionals keen to educate on the benefits of optimal cord clamping, believing in taking positive action through innovative collaboration. The BloodtoBaby modules being part of the collaborative work undertaken of which Hannah has taken the lead role.
Hannah's contribution to these modules centres on providing education about physiology of the newborn considering the impacts of obstetric and midwifery practice.
George Brooks
George has been a midwife for nearly 30 years in the North East England. He currently works as neonatal lead for a level I nurse-led neonatal unit, serving a maternity service that supports over 3000 women to give birth each year. In his role he leads neonatal resuscitation training for teams working in hospitals, midwife-led units and the community.
George's workplace has offered optimal cord clamping as standard practice since 2009 when obstetrician David Hutchon visited the unit to discuss how and why women's health professionals should provide care for the baby avoiding immediate cord clamping: David spoke physiological sense!
They have been fortunate enough to be able to source equipment so that they are able to offer intact cord resuscitation in all care settings so have extensive experience of intact cord resuscitation for babies born at varied gestation irrespective of mode of delivery.
Deborah Neiger
Debs Neiger has been a midwife for 20 years, 16 of those in independent practice. Deborah has always regarded optimal cord clamping as normal physiology and therefore normal for babies, while premature clamping has the potential for harm.
She has reflected this in her midwifery practise in the last two decades. Most of Deborah's practise and birth attendance is in a homebirth setting and this makes respecting physiology and optimal transition of the baby to extrauterine life even more crucial.
Deborah's contribution to this module is vital to ensure full scope perspective to educating about stabilisation with an intact cord for all babies in any setting.
Frequently Asked Questions
Get started now!

